Millions will lose health insurance starting Saturday. But they might not know it.
Tens of millions of men and women will start to eliminate their wellbeing insurance on Saturday, as five states start off the unwinding of a pandemic-era protection that held people today from currently being eradicated from the Medicaid rosters.
In the course of the general public wellbeing crisis, states ended up needed to continue to keep persons on Medicaid without the frequently annually reapplication system normally in spot. But now that the general public well being emergency is winding down, so are the Medicaid rolls.
“We are now in a position in just a few of times exactly where states can start to disenroll men and women — to redo their rosters for Medicaid — and this steady protection need is no for a longer period heading to be in put,” Dr. Avenel Joseph, vice president of plan for the Robert Wooden Johnson Foundation, informed ABC News.
The concern that Joseph and other advocates are worried about is that not adequate individuals know they are about to get kicked off their protection.
For Jeffrey Jackson, a 62-yr-previous Medicaid beneficiary in Arkansas who faces dropping that protection in a matter of days, that could be a “nightmare.”
Arkansas is a person of the five states that will get started taking away people today from coverage on April 1, together with Arizona, Idaho, South Dakota and New Hampshire.

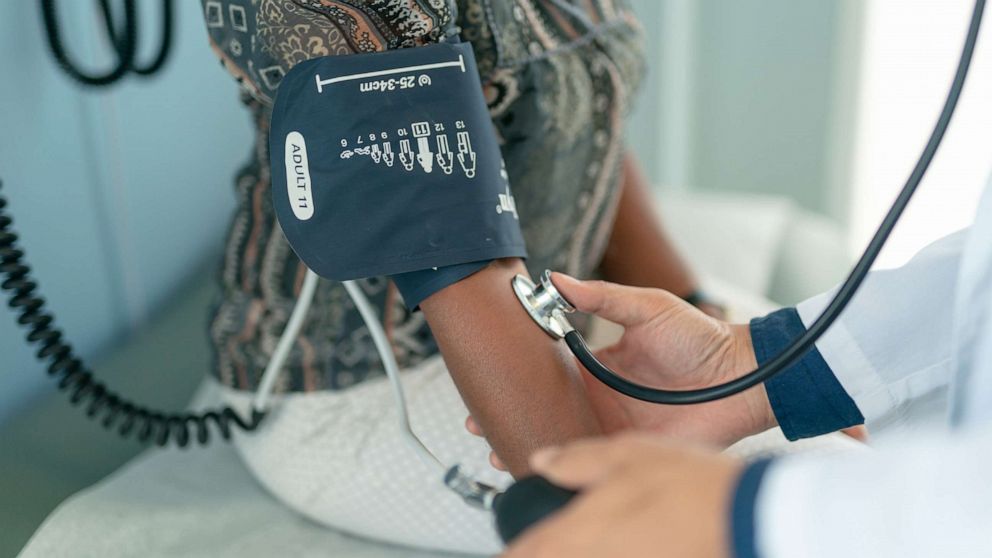
A lady sits on an examination table in a clinic while a health treatment qualified checks her blood force.
Stock Photograph/Getty Photographs
Without having Medicaid, Jackson’s economic selections would have to come down to “regardless of whether I would take in or regardless of whether I will get my treatment.”
Jackson reported he’ll have to meet up with with his medical practitioners to inquire them what drugs he can do with no.
“We’ll seem at what’s remaining and then I’ll say I will search at the value and what I can manage or won’t be able to afford,” Jackson told ABC Information.
Regardless of the dire stakes, losing Medicaid is a common trouble that employed to happen every year just before the pandemic — the normal man or woman on Medicaid acquired about 10 months of coverage a calendar year, for the reason that of something termed “churn,” which frequently takes place when bureaucratic hurdles drive folks out of the procedure for explanations as easy as lacking a letter in the mail or relocating.
According to estimates from KFF, a nonpartisan nonprofit that stories on nationwide overall health issues, around 65{bf0515afdcaddba073662ceb89fbb62b6b1bf123143c0e06b788e1946e8c353f} of men and women who do get disenrolled end up uninsured for a portion of the following yr.
Receiving again on wellness insurance policy can be difficult, Joseph mentioned.
“It’s not just like you check out a box and you can get again on Medicaid the subsequent working day. The procedure of having re-enrolled in Medicaid, even when you might be suitable, can just take months. And during that period of time of time, folks — folks but also their households, and children in specific — can slide as a result of the cracks,” Joseph stated.
The Office of Wellness and Human Providers estimates that this time all over, following a few many years with no “churn” in the system, around 7 million Us citizens who even now qualify for Medicaid will get rid of rewards.
An additional 8 million will get rid of coverage because they no longer qualify and need outreach to understand where they can enroll in other, reduced-value govt wellness plans through the Affordable Care Act, according to HHS.
“What we’ve heard from Medicaid directors across the states is this is the major shifting of insurance coverage for persons since the Very affordable Care Act was put in location over 10 a long time back,” Joseph said. “This is a significant endeavor.”
“And with that sort of movement,” Joseph said, “susceptible people will fall by way of the cracks.”






